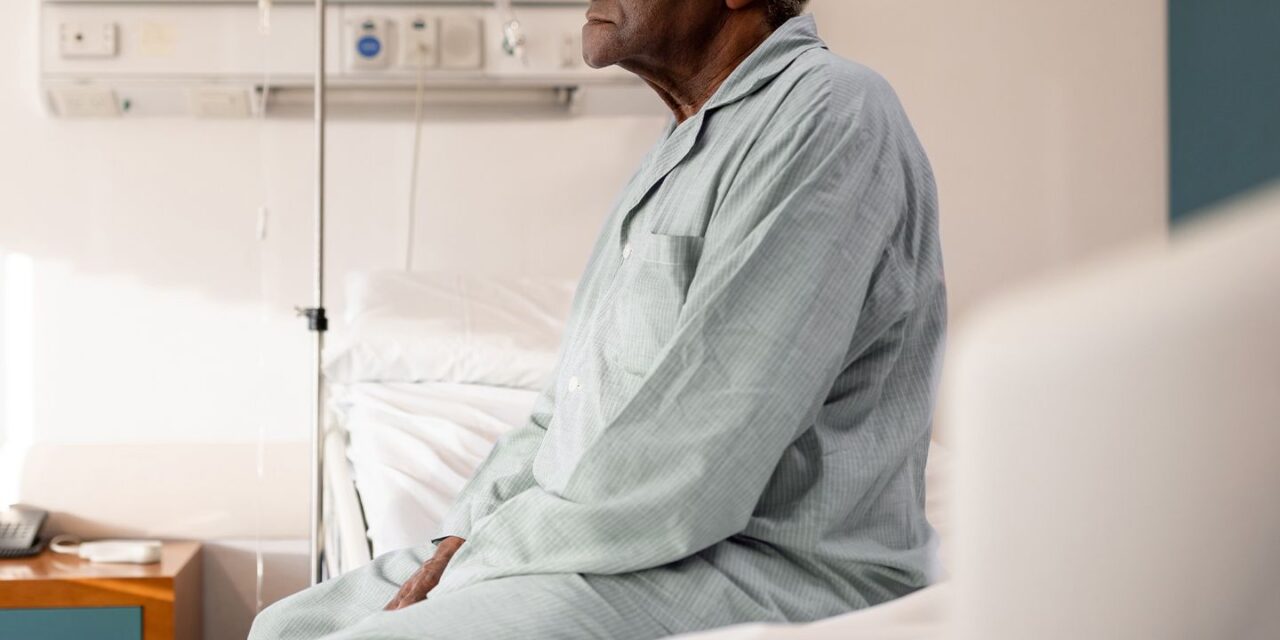
Older Black men are more likely to die within 30 days of surgery than any other subgroup of race and sex, according to a study published March 1 in the BMJ.
The inequality in death rate was the largest for elective surgeries, where the death rate of Black men was 50 percent higher than that of white men.
While a fair bit is known about such inequities, this study finds that it’s specifically Black men who are dying more, and they are dying more after elective surgeries, not urgent or emergent surgeries, said the lead study author, Dan Ly, MD, PhD, an assistant professor of medicine in the division of general internal medicine and health services research at the David Geffen School of Medicine at UCLA, in a press release.
“Our findings point to possibilities such as poorer pre-optimization of comorbidities prior to surgery, delays of care due to structural racism and physician bias, and worse stress and its associated physical burden on Black men in the United States,” said Dr. Ly in the release.
Unfortunately, these findings aren’t surprising. Racial disparities in healthcare have been well documented, and the data is becoming more granular over time, says Catherine McManus, MD, the surgical director of the thyroid biopsy program at Columbia University Irvine Medical Center in New York City, who was not involved in this study.
“I think a key point made in this particular study is noting the difference between elective and nonelective surgeries. The authors found that Black men had a higher postoperative mortality for elective procedures than white men, white women, and Black women. However, that difference in mortality disappeared when considering nonelective procedures,” says Dr. McManus.
There are two categories of surgery: elective surgery and urgent or emergency surgery, according to Johns Hopkins Medicine. An elective surgery doesn’t always mean an optional surgery. The term is used to describe any operation that can be scheduled in advance. The term elective is broad enough to encompass simple procedures such as mole removal or surgery for cancer or a heart condition.
Older Black Men Are 50 Percent More Likely to Die Than Older White Men
In previous studies, racial inequities in surgical care and outcomes, including a higher death rate after surgery for Black patients, have been well documented, according to the authors.
The new study is unique in that it separates race and gender and looks at elective versus nonelective surgeries.
Investigators used nationwide Medicare data collected between 2016 and 2018 on 1,868,036 adults with an average age of 75. Of those participants, 40.7 percent were white men, 53.4 percent were white women, 2.2 percent were Black men, and 3.7 percent were Black women. More than one million surgeries were performed, of which 70.3 percent were elective and 29.7 urgent or emergency.
Eight types of surgery were included in the analysis: abdominal aortic aneurysm repair, appendectomy, cholecystectomy, colectomy, coronary artery bypass surgery, hip replacement, knee replacement, and lung resection.
The researchers compared patient outcomes by race and sex among patients who received the same type of procedure at the same hospital.
To try to further isolate the potential effects of gender and race, researchers controlled for other factors that could influence the death rate 30 days postsurgery, including age, disability, and 27 different underlying chronic conditions.
They found that Black men had a higher death rate (3.05 percent) within 30 days of both urgent and elective surgery than white men (2.69 percent), white women (2.38 percent), and Black women (2.18 percent).
A similar pattern was found for elective surgery: Black men had a higher death rate (1.3 percent) than white men (0.85 percent), white women (0.82 percent), and Black women (0.79 percent).
This 0.45 percentage point difference between Black and white men for elective surgeries is pretty drastic, says Alejandro Garcia, MD, an assistant professor of surgery and the vice chair of diversity, equity, and inclusion at Johns Hopkins Medicine in Baltimore. “That’s a nearly 50 percent difference — that’s a lot,” he says.
Much of this difference persisted even when researchers compared patients who had been operated on by the same surgeon, the authors wrote.
The researchers did not find a statistically significant difference between Black and white men after urgent surgery, with death rates of 6.69 percent and 7.03 percent, respectively.
They did, however, find that deaths after urgent surgery were lower for both white and Black women than for men of either race, at 6.12 percent and 5.29 percent, respectively.
Social Factors May Be to Blame for the Disparity in Death Risk
These differences in postoperative mortality indicate that Black men do worse in more controlled operative settings where time and preparation are possible, and they fare the same as others in more urgent or emergent situations, says McManus.
“This finding illustrates the key point that there is nothing inherent about race or sex that leads to worse outcomes, but rather it is the social factors inherent to structural racism that are responsible for this disparity,” she says.
“Although the identification of the underlying mechanisms was beyond the scope of our study, there are several factors that can potentially explain the observed disparity in our study,” says a coauthor, Yusuke Tsugawa, MD, MPH, PhD, an associate professor of medicine at UCLA David Geffen School of Medicine in Los Angeles.
The structural racism that exists in the United States may at least partially explain the findings, he says. “For example, Black patients living in neighborhoods with predominantly Black residents tend to live close to hospitals that lack resources to provide high-quality healthcare,” says Dr. Tsugawa.
“It is interesting that these findings on the higher likelihood of postoperative mortality are very specific to Black males as opposed to Black individuals in general,” says Dr. Garcia.
“It is possible that Black men in particular face especially high cumulative amounts of stress and allostatic load, which refers to the cumulative burden of chronic stress and life events, potentially leading to a higher death rate after surgery among this population,” says Tsugawa.
A paper published in Psychotherapy and Psychosomatics in 2021 reviewed 267 studies that looked at the consequences of allostatic load and found that “allostatic load and overload are associated with poorer health outcomes.”
The Next Question: How to Fix the Problem
“Further research is needed to understand better the preoperative, intraoperative, and postoperative factors contributing to this higher mortality rate among Black men after elective surgery,” wrote the authors.
Future studies need to examine these findings on a more granular level, says McManus. “By looking at more patient-specific factors related to social determinants of health — education, income, insurance status — we may be able to further define where to direct our efforts and invest more resources to make healthcare more equitable for all individuals,” she says.
Garcia suggests that comparing these groups at each step in the continuum of care could reveal differences that could be addressed and improved.
“These findings are eye-opening — it’s important for surgeons as well as everyone in the public to see this,” says Garcia. “Awareness and action, on both on an individual and institutional level, is needed to begin to fix these complex problems.”